HEALTHY LIVING
It’s time to rethink heart health


(Family Features) On average, someone in the United States dies from cardiovascular disease (CVD) every 36 seconds, approximately 2,380 deaths each day, according to the American Heart Association. Each day, 405 deaths occur in the U.S. as the result of strokes, an average of one death every 3:33. More people die annually from CVD than from any other cause including cancer, COPD, diabetes, lung infections and the flu, according to the American Heart Association (AHA) 2021 Heart Disease and Stroke Statistics.
Consider these steps to #RethinkCVRisk to change the course of the disease and your life.
Understand Your Risk
COVID-19 has shown that those with underlying CVD face an especially high risk of serious COVID-19-related illness or even death, according to the Centers for Disease Control and Prevention (CDC). Regardless of whether you’ve received your COVID-19 vaccination, now is a good time to discuss your risk for heart disease with your doctor.
How Cardiovascular Disease Develops
Risk factors for CVD include high cholesterol, high triglycerides, diabetes and high blood pressure. Other factors that contribute to risk are family history, prior cardiovascular (CV) events, smoking, being overweight or obese and unhealthy diet and exercise habits. Over time, these risk factors can lead to injury of the blood vessel lining, causing inflammation, which can then trigger plaque growth. Plaque grows at different rates and in different arteries in the body for everyone and is often a slow, gradual process without symptoms.
As plaque buildup continues, the risk of suffering a CV event – such as heart attack or stroke – increases. If plaque ruptures, the body will try to repair the injury, potentially causing a blockage to form, and when an artery becomes fully blocked, blood flow is restricted. Blocked blood flow to the heart causes a heart attack while blocked blood flow to the brain causes a stroke.

Managing Risk Factors
The most effective way to prevent CVD is to understand and address risk factors. Triglycerides play an important role in heart health. Triglycerides store unused calories to give your body energy and are the most common type of fat in the body. They come from foods you eat such as butter, oils and other fats, as well as carbohydrates, sugars and alcohol. Your diet, lack of exercise, medical conditions, certain drugs and genetics can all cause high triglycerides.
In the past, medicines used to lower triglycerides, like fenofibrates and niacin, were commonly prescribed to help manage CV risk along with statins. However, clinical studies failed to show benefits and both the U.S. Food and Drug Administration (FDA) and American Diabetes Association discourage combining niacin and fenofibrates with statins.
Some turn to dietary supplement fish oil to help manage CV risk. However, supplements contain only 30% of the omega-3 fatty acids EPA and DHA (docosahexaenoic acid) with the majority of the product consisting of non-omega-3 ingredients, including saturated fats. Some data suggests certain ingredients in dietary supplement fish oils, such as DHA and saturated fats, may raise bad cholesterol.
While high triglycerides are an indicator of CV risk, lowering them won’t necessarily reduce your risk. However, addressing the underlying causes of high triglycerides can help, according to the AHA.
Treatment Options
With ongoing research, new standards-of-care are emerging. High cholesterol is a key CV risk factor with statins currently the first-line therapy for lowering cholesterol. Statins, diet and exercise can lower your CV risk by about 25-35%, but, for many people, controlled cholesterol doesn’t eliminate CV risk. This residual risk, or “persistent CV risk,” puts millions of patients at risk and has been the focus of therapeutic development for many years.
Talk with your doctor about FDA-approved options that can help further reduce your heart risk if you already take statins.
Truths and Falsehoods About Heart Disease Risk
1. Statins reduce your chance of experiencing a CV event by up to 90%.
False. Statins, diet and exercise can lower your risk by about 25-35%, but for many patients, controlled cholesterol doesn’t eliminate CV risk. This residual risk, or “persistent CV risk,” puts millions of patients at risk and has been the focus of therapeutic development for many years.
2. Managing high triglycerides along with taking statins is enough to reduce your risk.
False. High triglycerides are a CV risk factor but lowering them won’t necessarily reduce your risk. For example, earlier generation medicines prescribed to lower triglycerides, like fenofibrates and niacin, failed to show clinical benefit when used with statins to reduce CV risk. In fact, the FDA withdrew approval for fenofibrates and niacin in combination with statins because they add potential risk with no proven benefit to heart health.
3. Fish oil supplements are a proven way to get protection from a CV event.
False. Fish oil supplements are not FDA-approved medicines intended to treat or prevent a medical condition. Despite multiple clinical studies, these products have not been proven, to reduce CV risk on top of current medical therapies including statins.
4. Having a first CV event, such as a heart attack or stroke, puts you at greater risk to suffer another.
True. Having a CV event makes you more likely to suffer another. That’s why it’s important to protect against a first CV event or future events. To closely monitor your heart health, stay in close contact with your doctor and reduce your risk by keeping up with your medications, exercising and sticking to a healthy diet.
For more information about CVD and what you can do, look for #RethinkCVRisk on social media or visit truetoyourheart.com.
Photos courtesy of Getty Images
SOURCE:
Amarin Pharma, Inc.
HEALTHY LIVING
Getting high cholesterol under control

(Family Features) Heart disease is the nation’s leading cause of death for men and women, according to the Centers for Disease Control and Prevention, but many people aren’t aware they may be at elevated risk. More than 71 million adults in the United States have high low-density lipoprotein (LDL) cholesterol and nearly 50 million don’t have it under control, which puts them at higher risk for cardiovascular events, such as heart attack and stroke.
What’s more, nearly one-third (31%) of U.S. adults are not aware that having high cholesterol puts them at greater risk for heart attack and stroke, according to the findings of a recent study conducted by The Harris Poll commissioned by Esperion Therapeutics, Inc. The poll also revealed some inconsistent understanding about treatment options available for those with uncontrolled cholesterol. Fully 3 in 10 (30%) of those taking statins believe statins are the only LDL lowering treatment available for those with high LDL cholesterol.
“In auto racing, the red flag means danger on the track, stopping the race immediately,” said Dr. JoAnne Foody, chief medical officer at Esperion. “We are launching a patient education program, ‘Wave the Red Flag,’ to encourage people with uncontrolled high cholesterol to have their levels checked right away and discuss appropriate treatment options with their health care provider.”
If your high cholesterol is uncontrolled, understanding how you can achieve greater control can reduce your risk for serious health conditions, including potentially life-threatening cardiovascular events.
Consider these tips to get high cholesterol under control.
Talk with your doctor. Speaking with your physician is an important first step to managing any health condition. Your doctor can help you understand the severity of your condition and whether a treatment plan should be moderate or aggressive.
Check your progress. Keeping tabs on your cholesterol can help you and your health care team gauge whether your treatment plan is working. If you don’t have heart disease, you may not need to check as frequently, but your doctor can recommend the appropriate intervals to help manage your cholesterol most effectively.
Take medications as prescribed. Statins are the medications most often recommended by treatment guidelines for the management of blood cholesterol, and nearly one-third (30%) of those taking statins believe they are the only cholesterol-lowering treatment available, according to the survey. However, even with maximal statin therapy, some patients with chronic disease do not meet recommended LDL cholesterol levels. Taking your medications regularly and as instructed helps your doctor determine whether additional therapies – including non-statin treatments – could be useful to help manage your blood cholesterol.
Make lifestyle adjustments. Your diet plays a major role in lowering LDL cholesterol. Limiting fatty foods, especially those that are high in saturated and trans fats, is key. Monitoring your overall diet and exercising can also help reduce your risk of high cholesterol. Even if you don’t have high cholesterol, adopting more cholesterol-friendly habits can help prevent your levels from rising to unhealthy levels in the future.
To find additional information about managing your high cholesterol, talk to your health care provider and visit WaveTheRedFlag.info.
Fast Facts About Cholesterol
What is cholesterol?
The liver creates a fat-like waxy substance called cholesterol. It serves useful purposes for the body, including producing hormones and helping digest food.
How do you get high cholesterol?
The human body makes all the cholesterol it needs naturally, so any cholesterol you eat is cholesterol you don’t need. However, it can be difficult to avoid because you can find dietary cholesterol in many common foods, including meat, seafood, poultry, eggs and dairy. Other non-dietary contributing factors include health conditions like obesity and diabetes, as well as family history and advancing age.
What is a normal cholesterol level?
An average optimal level of LDL cholesterol is about 100 milligrams per deciliter (mg/dL).
An average optimal level of high-density lipoprotein, or HDL, cholesterol is at least 40 mg/dL for men and 50 mg/dL for women. HDL cholesterol can actually lower your risk of heart disease and stroke.
Are there symptoms of high cholesterol?
Unlike many health conditions, there are rarely any symptoms that your cholesterol is high. That’s what makes regular screening so important.
Photos courtesy of Shutterstock
SOURCE:
Esperion
HEALTHY LIVING
Learn CPR as a life-saving skill
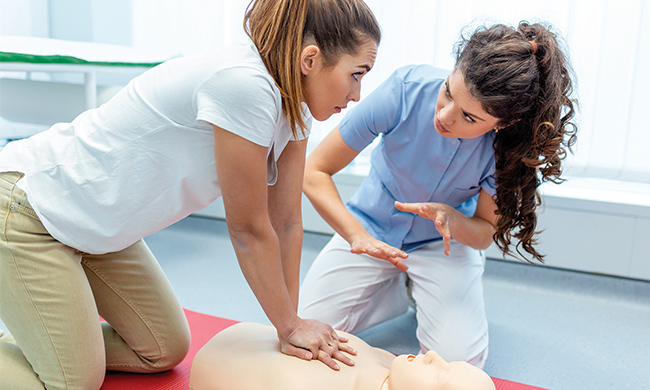
(Family Features) While many Americans agree Conventional CPR (cardiopulmonary resuscitation) or Hands-Only CPR (HOCPR) significantly improve a person’s chance of survival from cardiac arrest, less than half are confident they can perform either Conventional CPR or HOCPR in an emergency.
Black or Hispanic adults who experience cardiac arrest outside a hospital setting are substantially less likely to receive lifesaving care from a bystander. In spite of these survey results, the American Heart Association is working to change this by empowering members of these communities to learn lifesaving CPR, and a growing segment of respondents are willing to act in an emergency.
The American Heart Association’s 2023 survey also revealed that as a result of the organization’s efforts to change attitudes about performing CPR, which can lead to lifesaving results, more than half of African Americans said they would be willing to perform CPR in an emergency compared to 37% two years ago. Additionally, Hispanic and Latino respondents are more confident in their abilities to perform CPR.
Committed to turning a nation of bystanders into lifesavers, the American Heart Association’s multiyear initiative, Nation of Lifesavers, helps teens and adults learn how to perform CPR and use an automated external defibrillator (AED); share that knowledge with friends and family; and engage employers, policymakers, philanthropists and others to create support for a nation of lifesavers.
“Each of us has the power in our own hands to respond to a sudden cardiac arrest,” said Anezi Uzendu, M.D., American Heart Association expert volunteer. “We simply need to know what to do and have the confidence to act.”
The long-term goal: to ensure that in the face of a cardiac emergency, anyone, anywhere is prepared and empowered to perform CPR and become a vital link in the chain of survival, aiming to double the survival rate of cardiac arrest victims by 2030. It takes just 90 seconds to learn how to save a life using HOCPR, which can be equally as effective as traditional CPR in the first few minutes of cardiac arrest.
Nationally supported by the Elevance Health Foundation, the American Heart Association’s HOCPR campaign is focused on chest compression-only CPR. If a teen or adult suddenly collapses due to a cardiac event, you can take two steps to save a life: immediately call emergency services and use these tips to begin performing HOCPR.
- Position yourself directly over the victim.
- Put the heel of one hand in the center of the chest and put your other hand on top of the first.
- Push hard and fast in the center of the chest at a rate of 100-120 beats per minute, which is about the same tempo as the song “Stayin’ Alive” by the Bee Gees, and at a depth of approximately 2 inches.
- Continue compressions and use an AED, if available, until emergency help arrives.
To learn more about how you could be the difference between life and death for someone experiencing a cardiac event, visit Heart.org/nation.
Photo courtesy of Shutterstock
SOURCE:
American Heart Association
HEALTHY LIVING
Combating loneliness in older adults

(Family Features) The bonds found in friendships and other relationships are an important factor in health and wellness – even science says so.
According to the American Psychological Association, forming and maintaining social connections at any age is one of the most reliable predictors of a healthy, happy and long life. Studies show having strong and supportive friendships can fend off depression and anxiety, lower blood pressure and heart rates in stressful situations and change the way people perceive daunting tasks.
 However, statistics show approximately half of U.S. adults lack companionship and feel socially disconnected, according to the U.S. Surgeon General’s Advisory on the Healing Effects of Social Connection and Community. In fact, 12% don’t have anyone they consider a close friend, per the Survey Center on American Life. This “epidemic of loneliness,” as coined by U.S. Surgeon General Dr. Vivek Murthy, can take a severe toll on mental and physical health.
However, statistics show approximately half of U.S. adults lack companionship and feel socially disconnected, according to the U.S. Surgeon General’s Advisory on the Healing Effects of Social Connection and Community. In fact, 12% don’t have anyone they consider a close friend, per the Survey Center on American Life. This “epidemic of loneliness,” as coined by U.S. Surgeon General Dr. Vivek Murthy, can take a severe toll on mental and physical health.
As people age, the risks of isolation increase. With America’s older population growing rapidly – the 65 and older population reached more than 55 million in 2020 – discussing how older adults can combat loneliness is relevant to public health and individual well-being.
Consider volunteering, which is one of the best and most rewarding ways to combat loneliness.
Volunteering Combats Loneliness
People often volunteer to find a sense of purpose, learn new skills, improve their communities or establish new routines after retiring or becoming empty nesters. For many, making friends through volunteer work is a welcome bonus. The act of volunteering provides proven benefits for older adults.
Forming connections can make all the difference in a person’s volunteer experience and sense of well-being. People who meet through volunteer work inherently share a common interest and something to bond over. These friendships can carry over outside of volunteer work and lead to bonding over other hobbies and interests.
Connection-Focused Volunteer Opportunities
In addition to making friends with fellow volunteers, many older adults also form relationships with the people they’re serving, especially if those recipients are their peers.
For example, AmeriCorps Seniors is the national service and volunteerism program in the federal agency of AmeriCorps that connects adults aged 55 and up to local service opportunities that match their interests. Its Senior Companion Program pairs volunteers with other older adults or those with disabilities who need companionship or assistance. Volunteers may help with tasks such as paying bills, shopping or getting companions to appointments. In some cases, volunteers may also provide support and respite for family members caring for loved ones with chronic illnesses.
“We often think of volunteering as ‘giving back,’ but we’ve seen firsthand that it often becomes so much more than that,” said Atalaya Sergi, director of AmeriCorps Seniors. “By spending a few hours each week with another older adult in need of support, our volunteers are not only giving back to others, but they’re adding meaning to their own lives and establishing new connections. They’re helping to fight the loneliness epidemic one visit at a time.”
Growing older can come with challenges, but some of those can be minimized with a positive mindset and commitment to remaining connected and engaged – whether with friends, relatives or fellow community members. Fostering relationships is a key ingredient to a healthier and more fulfilling life.
For more information and to find volunteer opportunities near you, visit AmeriCorps.gov/YourMoment.
Meet Friends Who Connected Through Service
 Ray Maestas felt unfulfilled post-retirement and began volunteering with the AmeriCorps Seniors Senior Companion Program. He was connected with Bob Finnerty, a man with blindness looking for assistance a few days each week. They quickly struck up a routine of errands, reading and conversation that’s since become a friendship they both cherish.
Ray Maestas felt unfulfilled post-retirement and began volunteering with the AmeriCorps Seniors Senior Companion Program. He was connected with Bob Finnerty, a man with blindness looking for assistance a few days each week. They quickly struck up a routine of errands, reading and conversation that’s since become a friendship they both cherish.
“The Senior Companion Program has provided an avenue to enrich the lives of not only the participants but the people who are volunteering,” Maestas said. “Bob and I have gotten to the point where he’s a very important part of my life.”
Finnerty echoed those sentiments and shared his own appreciation for Maestas’ friendship.
“I’ve always relished my independence and I feel Ray is not just a person who reads for me – he’s a friend,” Finnerty said.
In the last few years, Maestas moved and now serves with a different chapter of the Senior Companion Program. He and Finnerty keep in touch. Maestas said they talk about every third day.
SOURCE:
AmeriCorps Seniors
-

 NEWS1 year ago
NEWS1 year ago2 hurt, 1 jailed after shooting incident north of Nocona
-

 NEWS5 months ago
NEWS5 months agoSuspect indicted, jailed in Tia Hutson murder
-

 NEWS12 months ago
NEWS12 months agoSO investigating possible murder/suicide
-

 NEWS1 year ago
NEWS1 year agoWreck takes the life of BHS teen, 16
-
 NEWS9 months ago
NEWS9 months agoMurder unsolved – 1 year later Tia Hutson’s family angry, frustrated with no arrest
-

 NEWS12 months ago
NEWS12 months agoSheriff’s office called out to infant’s death
-

 NEWS1 year ago
NEWS1 year agoBowie Police face three-hour standoff after possible domestic fight
-

 NEWS1 year ago
NEWS1 year agoDriver stopped by a man running into the street, robbed at knifepoint





