Live Better
SMA and the new miracle drug Spinraza
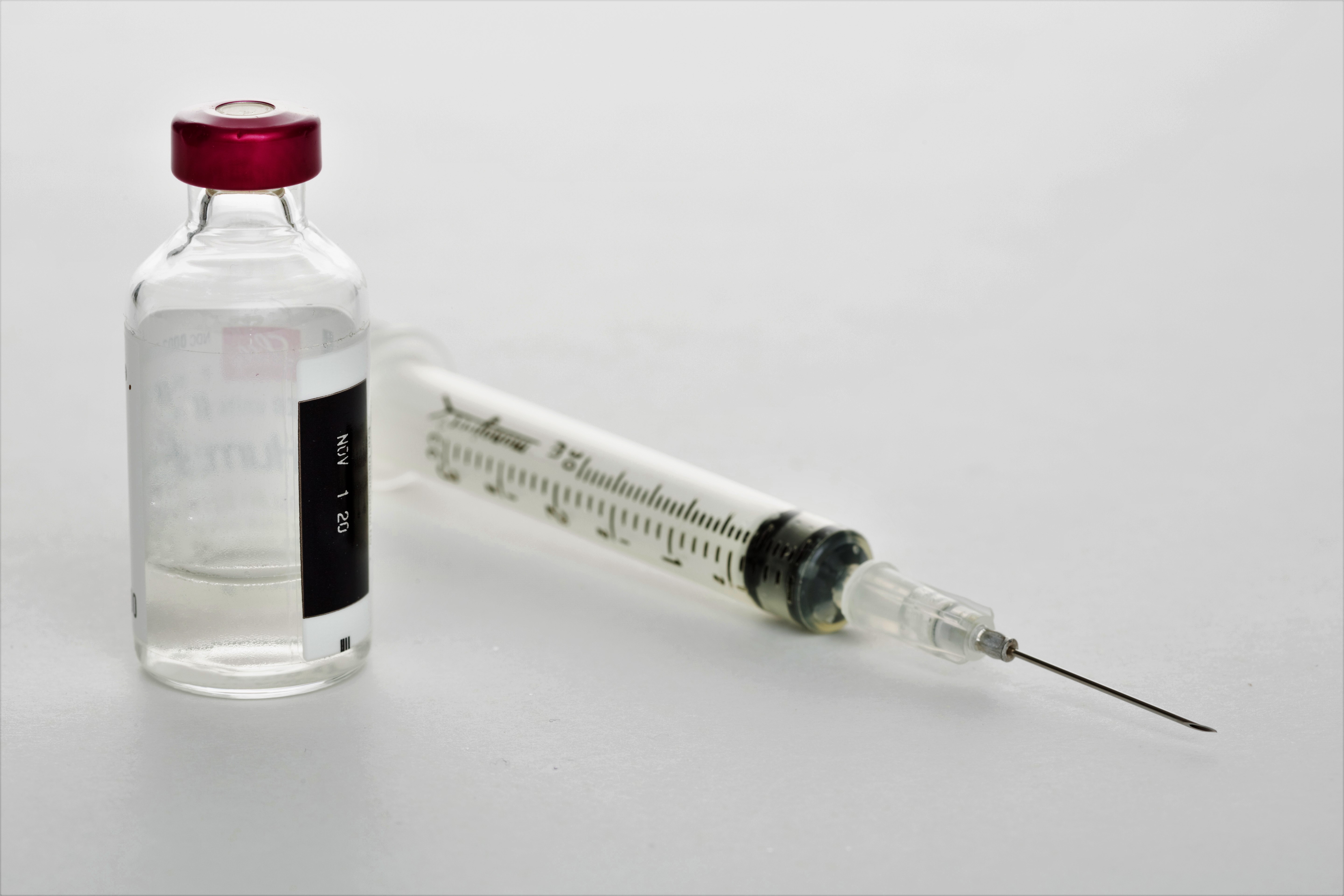
Spinal muscular atrophy, or SMA, is a genetic disease that attacks nerve cells in the spinal cord. These nerve cells, known as motor neurons, communicate with the voluntary muscles in the body, such as those in the arms and legs. As more neurons are lost, muscles start to weaken and breathing, crawling, swallowing, and walking can become more difficult. It also can be difficult for those with SMA to control movements in their heads and necks. Though SMA runs in families, parents can exhibit no symptoms but still carry the gene. There are many types of SMA, and, according to the National Institute of Neurological Disorders and Stroke, the type of SMA is determined by the age of onset and the severity of symptoms. SMA Type I is evident at birth or within the first few months of a child being born. Symptoms may include difficulty swallowing, feeble movements of the arms and legs, loose limbs and trunk, impaired breathing, and a weak sucking reflex. SMA Type II is evident between the ages of six and 18 months, and the legs are typically more impaired than the arms. An early indicator may be a baby who is not crawling or walking. SMA Type III may be evident when a child reaches his or her toddler years, but sometimes does not appear until adolescence. When a child has SMA Type III, he or she may have trembling fingers and may experience difficulty getting up from a sitting position. Children with SMA Type II or Type III are at an increased risk of respiratory infections.
What causes SMA?
According to the Muscular Dystrophy Association, chromosome 5 SMA, the most common form of SMA, is caused by a deficiency of SMN, a motor neuron protein. This protein is necessary for normal motor neuron function, and a deficiency of SMN is caused by mutations on chromosome 5 in the SMN1 gene. Mutations in other genes may also cause SMA, and such cases are referred to as non-chromosome 5 SMA.
What are the symptoms of SMA?
There are various types of SMA, and the symptoms can vary depending on the type of SMA a person has. The following are some of the symptoms associated with the various types of SMA.
- Type 1: Type 1 is the most severe type of SMA. When a child is type 1, he or she may have difficulty supporting his or her head and sitting without help. Difficulty swallowing and weakness in the arms and legs may also occur. The muscles that control breathing also can be compromised when a child has type 1 SMA, and breathing problems can affect a child’s life expectancy.
- Type 2: Type 2 SMA typically affects the legs more than the arms. Type 2 SMA affects children between six and 18 months of age, and such kids may be able to sit, stand or walk with help.
- Type 3: The mildest form of SMA, type 3 may be referred to as juvenile SMA. Children with type 3 can often stand or walk without help, but they may have difficulty climbing stairs, getting up from a chair or running.
- Type 4: Type 4 SMA begins in adulthood, and men and women may experience muscle weakness, twitching or breathing problems. Physical therapy can help men and women better manage their symptoms, which typically only affect the upper arms and legs.
Recently the FDA approved an amazing new drug Spinraza to treat symptoms of SMA and prolong these life of individuals taking Spinraza. With a few injections, patients with SMA may be able to gain muscle strength and live longer by a year or more. It cost $125,000 an injection, and in the first two months one takes 4 injections in the spine. That’s half a million dollars for the first four shots. Subsequent costs for this possibly lifelong therapy are expected to be about $375,000 annually, with about three injections required each year. While this may seem extremely expensive the drug was developed to save lives, along with some resources available to help individuals requiring the drug. With coverage being more readily available to those effected the most, starting with SMA type I. Remember if you are trying to obtain Spinraza use every resource available at your disposal and educate yourself on the drug, available resources, and your healthcare. Don’t be afraid to ask questions and challenge your neurologist who would prescribe Spinraza along with your insurance representative, and if you have to, seek out a social worker for assistance. Be your own advocate. Take into account this drug has been developed and approved in a significantly short amount of time. Spinraza is for a relatively low percentage of the population, lots of money and resources were put into the development of this drug. For more information and resources go to SMAnewstoday.com. Remember to connect yourself with other individuals with SMA to share resources and connect with others who are going through the same thing you may be experiencing with SMA.
Parents can also learn more about SMA by visiting the Muscular Dystrophy Association online at www.mda.org & www.curesma.org
Live Better
Ready, set, spring: 5 early season yard tips

(Feature Impact) As the days lengthen and warm air has you ready to get your patio furniture out of storage, that means it’s time to give your yard a fresh start. With a little planning now, you’ll be rewarded with a fuller, greener and easier-to-maintain outdoor space once spring is in full bloom.
1. Start With a Clean Slate
Winter leaves behind plenty of debris, including fallen branches and matted leaves. Before you start planting, take a walk around your yard and tidy up:
- Rake moisture-trapping twigs and leaves that can cause fungus
- Remove dead plants or spent annuals from flower beds
- Sweep or power wash patios and walkways
2. Tune Up Tools
Digging into yard work only to find rusty shears or a squeaky mower can prolong the task. Instead, ensure your tools are in good working order:
- Sharpen blades on lawn mowers, shears and pruners
- Install fresh string on trimmers and weed eaters
- Replace old fuel or clean air filters on gas-powered tools
3. Assess Your Lawn
Early spring is ideal for noticing how winter treated your grass. Dethatching and aeration can go a long way toward helping grass absorb nutrients. Set the stage for lush growth once warmer weather arrives by looking for:
- Bare patches that need reseeding
- Weeds making an early debut
- Compacted soil where water pools instead of soaking in
4. Give Plants the Right Start
Now’s the time to prep beds for new life. Before you plant:
- Loosen soil and mix in compost for nutrients
- Add mulch around perennials
- Plan your planting based on sun and shade patterns
5. Hydrate Wisely
Strong roots start with proper hydration. Even before sprigs pop up, early spring can be dry as the sun gets higher. Remember to:
- Water flowerbeds if rainfall has been scarce
- Check irrigation systems for damage
- Mulch lightly after soil warms to lock in moisture
Getting your yard ready early in spring isn’t about perfection; it’s about setting yourself up for outdoor enjoyment all season long. Find more tips to get your yard in shape at eLivingtoday.com.
Photo courtesy of Shutterstock
SOURCE:
Live Better
Refresh your home: Spring cleaning checklist

(Feature Impact) After months of winter, spring cleaning isn’t just about dusting and vacuuming – it’s about inviting sunlight and fresh air into your space through the open windows and giving yourself a fresh start for the longer days ahead.
It’s also a perfect opportunity to clear out the old and make room for new experiences, memories and energy. Whether you’re tackling deep cleaning for the first time or you have seasonal rituals for tidying up your home, this room-by-room guide can help you plan and conquer seasonal chores.
Whole Home:
- Declutter spaces: Donate, recycle or discard what you don’t need
- Wash windows inside and out
- Dust baseboards, walls, vents and ceiling fans
- Wipe down doors, knobs and light switches
- Vacuum and clean under and behind furniture
- Clean curtains and blinds
- Store seasonal items like winter clothing and decor
- Replace air filters
- Shampoo carpet
Kitchen:
- Empty and wipe down refrigerator and freezer
- Clean oven, stovetop and microwave
- Scrub countertops and backsplashes
- Clean out the garbage disposal
- Sweep and mop floors
- Organize the pantry and throw away any expired items
Bathrooms:
- Scrub grout and tile
- Clean mirrors and glass surfaces
- Deep clean toilets
- Wipe down cabinets and bathroom fixtures
- Wash rugs, floor mats and the shower curtain and liner
- Empty trash and clean the bin
Bedrooms and Other Living Areas:
- Wash bedding, pillows and linens
- Organize closets and drawers
- Vacuum chair, couches and mattresses as well as under cushions
- Dust shelves and decor
- Clean light fixtures and lampshades
Outdoor Areas:
- Power wash patios, sidewalks and driveways
- Wipe down outdoor furniture and replace textiles like pillows, cushions and umbrellas
- Clear debris from garden beds
- Prune shrubs, plants and trees
- Organize garages and sheds
- Reconnect hoses and sprinklers
- Prep lawn equipment such as mowers, weed eaters and blowers
For more spring cleaning tips and tricks, visit eLivingtoday.com.
Photo courtesy of Shutterstock
SOURCE:
Live Better
Curating a memorable vacation for your family

(Family Features) Travel has a way of slowing time down, creating memories for loved ones that last long after suitcases are unpacked and regular routines return. For many Americans, their most treasured family memories took place on a vacation or trip rather than at home.
In fact, nearly 67% said they value a core memory more than a physical souvenir after a vacation, according to a survey commissioned by Holland America Line, a cruise line that has been exploring Alaska for nearly 80 years. What’s more, almost 86% of survey respondents said they have looked at photos or videos from a past trip to lift their mood, and more than 90% said positive travel memories can improve their mood during difficult times.
With Alaska on the travel bucket list of more than two-thirds of Americans, it’s a destination that is influencing experience-focused family adventures.
 Explore Curiosities
Explore Curiosities
Travel is about more than seeing new places. For many Americans, it’s also a time to learn, explore new interests and slow down. Booking a cruise can encourage those behaviors.
According to the survey, 61% of Americans are more likely to try new foods while traveling on a cruise, and nearly half (48%) said they’ve discovered a new interest or hobby during their cruise, including wildlife, food, history or culture. For example, cruise guests may be able to try local specialties, like fresh Alaskan seafood, reindeer sausage, birch syrup and Alaskan berries, while on board.
Unstructured time is part of the appeal of cruises, with 28% of respondents sharing they read more during their trips.
Focus on Nature
Nature-focused destinations stand out because they offer experiences that feel rare and immersive, especially in places where wildlife and landscapes are central to the journey. More than 4 in 10 survey respondents said seeing wildlife in nature would be the most memorable family vacation experience, compared with about 12% who said meeting a character at a theme park would stand out most.
Whether spotting whales, watching glaciers calve or seeing the Northern Lights stretch across the Alaskan sky, the landscape being part of the experience helps define the journey. To help guests witness the majestic animals found in Alaska, including whales, eagles, bears, moose, otters, seals, sea lions and more, Holland America Line carries a wildlife expert on board. Plus, a wildlife spotting guide points out native animals found along the cruise route and a map with the best places to see each species is included.
“Guests tell us time and again how profoundly nature shapes the memories they carry home,” said Robert Morgenstern, senior vice president of Alaska Operations at Holland America Line. “Wildlife sightings, time outdoors and shared moments linger long after the cruise ends, especially for families exploring Alaska together.”
Reimagine Family Time
For families, travel often creates time for bonding that daily routines simply don’t allow. More than half of the survey respondents said their best family memories occurred while traveling together, and more than 4 out of 5 (82%) said some of their strongest family bonding moments happened during a vacation or family trip.
In addition to shared memories, more than 91% said travel had a positive impact on their mental and emotional well-being.
As travelers look for relief from routine and overstimulation, finding experiences rooted in nature, exploration and shared moments can help create lasting memories and emotional connection.
To learn more about Alaska travel and book your next family adventure, visit hollandamerica.com.
SOURCE:
-

 NEWS3 years ago
NEWS3 years agoSuspect indicted, jailed in Tia Hutson murder
-

 NEWS4 years ago
NEWS4 years ago2 hurt, 1 jailed after shooting incident north of Nocona
-

 NEWS3 years ago
NEWS3 years agoSO investigating possible murder/suicide
-

 NEWS3 years ago
NEWS3 years agoWreck takes the life of BHS teen, 16
-
 NEWS3 years ago
NEWS3 years agoMurder unsolved – 1 year later Tia Hutson’s family angry, frustrated with no arrest
-

 Show us something good9 years ago
Show us something good9 years agoCountry music star children perform in Bowie
-

 NEWS3 years ago
NEWS3 years agoSheriff’s office called out to infant’s death
-

 100th Birthday4 years ago
100th Birthday4 years agoLooking back at the 1958 Centennial edition of The Bowie News










