HEALTHY LIVING
Stay safe, healthy during and after emergencies

4 tips to prepare for natural disasters that can negatively impact physical and mental health
(Family Features) As you’re making your emergency preparedness checklist, it’s also important to protect your heart and overall health in the wake of a hurricane, tornado or other natural disaster.
The experts at the National Oceanic and Atmospheric Administration predict an above-average Atlantic Ocean hurricane season for the seventh year in a row. Research shows it’s not only physical devastation that impacts the health and safety of people in the path of a natural disaster.
In fact, in a study presented at the American Heart Association’s Epidemiology, Prevention, Lifestyle and Cardiometabolic Health 2021 Scientific Sessions, researchers found there were higher rates of high blood pressure, obesity and pre-diabetes among survivors of Hurricane Maria in Puerto Rico in 2017, as well as increased incidences of heart disease and stroke two years after the storm compared to two years prior to the hurricane.
It’s not only hurricanes that can have a negative impact on cardiovascular health. A study published in the journal “Hypertension” found a significant increase in blood pressure levels and the incidence of high blood pressure among people who were forced to evacuate following the Great East Japan Earthquake in 2012.
Gustavo E. Flores, M.D., a member of the American Heart Association’s Emergency Cardiovascular Care committee, said there are several factors that may lead to increased cardiovascular disease and risk after a natural disaster.
“During and after a storm, many people experience extreme stress and trauma, which research shows can lead to an increase in cardiovascular disease risk,” he said. “The impact can be more intense for heart disease and stroke patients. Additionally, in the aftermath of a significant natural disaster, property destruction and evacuations affect many basic support resources. This can make it challenging to see a health care professional for routine check-ups or refill or adjust medications, especially for more vulnerable populations.”
Flores, chairman and chief instructor for Emergency & Critical Care Trainings, LLC, said it’s important for people to be prepared and plan ahead. Consider these quick tips from Flores and the American Heart Association, which is celebrating 100 years of lifesaving service as the world’s leading nonprofit organization focused on heart and brain health for all:
- Take time to write down any medical conditions, allergies and medications, including doses and the time you take medications, along with your pharmacy name, address and phone number. Keep the information with any other “go-kit” items you have handy for quick evacuation.
- If you need to evacuate, even temporarily, bring your medications and health information with you in a resealable plastic bag to help keep it dry.
- If your medication is lost, damaged by water or was left behind when you evacuated, research open pharmacies and seek a refill as quickly as possible. Some states allow pharmacists to make medically necessary exceptions on certain types of prescription refills during an emergency.
- Use the Patient Preparedness Plan if you have diabetes and use insulin. There you’ll find a checklist of supplies and guidelines to prepare for an emergency.
Another way to prepare for a possible medical emergency is to learn how to perform hands-only cardiopulmonary resuscitation (CPR) and how to use an automated external defibrillator until help arrives. If performed correctly, CPR can double or triple a person’s chance of survival.
Visit Heart.org for the latest on heart health and the Disaster Resources page for a wide range of helpful information.
Photo courtesy of Shutterstock
SOURCE:
American Heart Association
HEALTHY LIVING
Understanding the hidden dangers of LDL (Bad) Cholesterol

(Family Features) These days, wellness information is practically everywhere you turn. Do this; don’t do that. Eat more of this; eat less of that. This is good for you; that is bad.
It can be hard to cut through all the noise, but the reality is, when it comes to something as serious as your heart health and LDL cholesterol – the “bad” cholesterol – ignoring it can be downright dangerous for your health.
According to the American Heart Association, about every 40 seconds, someone in the United States has a heart attack, and strokes occur at about the same frequency.
High LDL cholesterol, often called “bad” cholesterol, significantly increases your risk of heart disease.
A poll conducted by The Harris Poll for the American Heart Association revealed 75% of heart attack and stroke survivors reported having high cholesterol. Yet nearly half (47%) of heart attack and stroke survivors are unaware of their LDL cholesterol number. This lack of awareness shows more knowledge is needed to help survivors proactively manage their health.
In fact, knowledge is key to reducing your risk of heart disease. Understanding the impact of LDL cholesterol and knowing your LDL number can help you make informed decisions.
Cholesterol: The Good and The Bad
Cholesterol is a waxy, fat-like substance your body needs to build cells and produce hormones. However, not all cholesterol is created equal:
- LDL (low-density lipoprotein) Cholesterol: This is the “bad” cholesterol. When too much LDL cholesterol circulates in the blood, it can build up in the inner walls of the arteries that feed the heart and brain, forming plaque that can narrow and eventually block these arteries, leading to heart attack or stroke.
- HDL (high-density lipoprotein) Cholesterol: Known as the “good” cholesterol, HDL helps remove the “bad” cholesterol from the arteries, protecting against heart attack and stroke.
A Silent Threat
Many people think high cholesterol has obvious signs, but that’s not always the case. In fact, about half of U.S. adults and 42% of heart attack and stroke survivors mistakenly believe high cholesterol has clear symptoms. However, high LDL cholesterol typically doesn’t show any signs, which is why it’s known as a silent threat to your heart.
People who have had a heart attack or stroke are at higher risk of future cardiovascular problems, which is why it’s important to monitor your cholesterol regularly to help prevent future events.
It’s also important to know high LDL cholesterol can be genetic, meaning someone who eats a healthy diet and exercises regularly can still have high cholesterol. Additionally, the risk of high LDL cholesterol increases with age.
That’s why the American Heart Association’s “Lower Your LDL Cholesterol Now” initiative, nationally sponsored by Amgen, emphasizes the importance of regular cholesterol checks regardless of your weight, diet and physical activity levels. Knowing your LDL cholesterol number – and understanding the target levels based on your health history – gives you the opportunity to manage your health proactively. This enables you to make informed decisions to prevent future heart issues.
Know Your Number
You can reduce your risk of a heart attack or stroke by knowing and addressing your LDL cholesterol number.
Working closely with your doctor allows you to actively manage high LDL cholesterol – often a key risk factor you can help control – and together, you can develop a personalized treatment plan. Ask your doctor or health care provider for a cholesterol test to know your LDL number. Understanding your cholesterol number is the first step toward managing it effectively. If necessary, appropriate management of your LDL cholesterol can help reduce your risk of a heart attack or stroke.
Your doctor may also talk with you about your personal and family medical history; previous heart-related medical events such as a heart attack or stroke; lifestyle habits such as tobacco use, obesity, unhealthy living or aging; racial and ethnic backgrounds; and reproductive health.
Lower is Better
When it comes to your cholesterol, guidelines from the American Heart Association and the American College of Cardiology recommend “lower is better” to reduce your risk. Studies show that an LDL number or below 100 mg/dL is ideal for healthy adults.
If you have a history of heart attack or stroke and are already on a cholesterol-lowering medication, your doctor may aim for your LDL to be 70 mg/dL or lower.
Talk to your doctor about the right treatment plan for you. Positive lifestyle habits, such as exercising and eating a healthy diet, may also help.
However, if you’ve had a heart attack or stroke before, lifestyle changes alone may not be enough to lower your risk of another event. Your doctor may recommend cholesterol-lowering medications to protect your heart health.
Learn more about LDL (bad) cholesterol by visiting heart.org/LDL.
SOURCE:
HEALTHY LIVING
Save a life from stroke

(Family Features) Strokes can happen to anyone, at any age – even young people. Despite being one of the leading causes of death and long-term disability in the United States, strokes are largely preventable, treatable and beatable – if you can control your risk factors.
According to the American Stroke Association, a division of the American Heart Association, every 40 seconds, someone in the U.S. has a stroke. Keeping blood pressure in check, living a healthy lifestyle and knowing stroke warning signs may help protect you and your loved ones.
Here are key insights from the American Stroke Association’s Together to End Stroke initiative, nationally supported by the HCA Healthcare Foundation.
Controlling Risk Factors
Up to 80% of strokes may be preventable, according to the American Stroke Association. You can take action to prevent strokes by managing your risk factors, like high blood pressure, a leading cause and controllable risk factor for stroke and heart disease.
Other risk factors include diabetes and obesity, which can be kept in check with healthy lifestyle behaviors such as good nutrition. Quitting smoking and being physically active are important. Atrial fibrillation, or AFib, which is a quivering or irregular heartbeat, also increases stroke risk. In fact, people with AFib are five times more likely to have a stroke, according to the American Heart Association.
Preventing a Second Stroke
Nearly 1 in 4 strokes occur in people who had a previous stroke, sometimes because they don’t know what caused the first, making identifying the cause of the stroke a key step toward future prevention. Treatment depends on the type of stroke someone is having, which can be determined with a series of medical evaluations and tests.
Work with your health care professional to develop a plan that helps you move forward after a first stroke while preventing a second. This plan should include controlling risk factors, like achieving and maintaining healthy blood pressure, blood sugar and cholesterol levels.
“Preventing a second stroke is possible with the right approach,” said Teresita Casanova, MD, HCA Healthcare affiliated neurologist and American Stroke Association volunteer expert. “Taking medicines as prescribed, monitoring health numbers, and making small, consistent lifestyle changes can make a big difference. Stroke survivors should feel empowered to take control of their health and work with their care team to build a strong prevention plan.”
To help you in your journey, you can rely on tools such as the Heart & Stroke Helper, a free self-management app available for stroke survivors and their caregivers. The app allows patients to oversee their health in one place with features that track progress on lifestyle habits, manage medications, track health numbers, provide information about stroke and allow patients to connect with others for inspiration.
Find more ways to manage second stroke risk at Stroke.org

Act F.A.S.T.: How to Detect Signs of Stroke
Most adults in the U.S. don’t know the stroke warning signs, nor that stroke is largely treatable if you call 911 as soon as you recognize the symptoms.
Learning the acronym F.A.S.T. can help you recognize that someone may be having stroke symptoms so you can take life-saving action.
F: Face Drooping. Does one side of the face droop, or is it numb? Ask the person to smile. Is the person’s smile uneven?
A: Arm Weakness. Is one arm weak or numb? Ask the person to raise both arms. Does one arm drift downward?
S: Speech. Is speech slurred? Is the person unable to speak or hard to understand? Ask the person to repeat a simple sentence, like “The sky is blue.”
T: Time to Call 911. If you or anyone else shows any of these symptoms, call 911 immediately.
Photo courtesy of Shutterstock
SOURCE:
HEALTHY LIVING
How to conduct a skin care self-exam
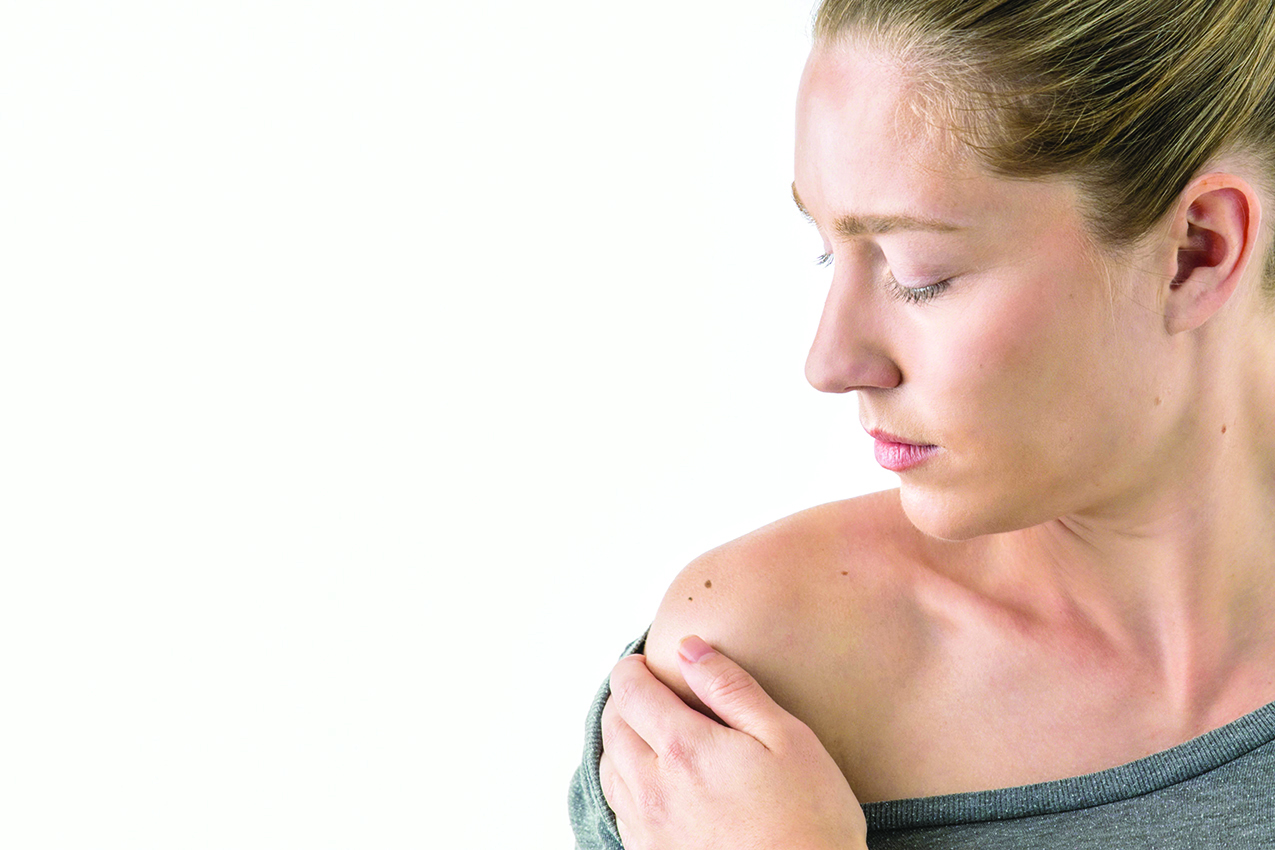
Time spent soaking up the summer sun is one of the things that makes the season so appealing. Warm outdoor air has a calming effect that can make anyone feel more relaxed and comfortable.
As good as warm summer sun can feel, overexposure to the sun can be dangerous. The World Cancer Research Fund reports there were more than 330,000 new cases of skin cancer diagnosed across the globe in 2022. A significant percentage of skin cancer cases can be prevented, and prevention is a multifaceted process that includes skin care self-examinations. Self-exams do not take up much time, and individuals can speak with their physicians about how frequently they should check their skin for signs of skin cancer. The U.S. National Library of Medicine offers the following instructions for how to conduct a skin self-exam.
Choose the right time to examine your skin. The USNLM recommends conducting a skin exam after bathing. Women who routinely conduct breast self-exams can check their skin at this time as well.
Use a full-length mirror. ItÕs not always easy to examine skin throughout the body. But signs of skin problems can occur anywhere on the body, including areas that might be hard to see without help. If possible, conduct a self-exam of the skin in front of full-length mirror in a brightly lit room.
Identify what youÕre looking for. The USNLM notes you should be looking for any new skin markings. This includes bumps, moles, blemishes, and changes in skin color.
Pay close attention to preexisting moles. A potential sign of skin cancer includes moles that change over time. Examine preexisting moles to see if they have changed in size, texture, color, and shape.
Look for unusual moles. The USNLM characterizes certain moles as Òugly duckling moles.Ó These unique moles look and feel different from nearby moles and may be indicative of skin cancer. Speak with a dermatologist if a self-exam uncovers the presence of moles with uneven edges or differences in colors or asymmetric shapes. Moles that look different from one side to the other also should be brought to the attention of a dermatologist. Moles that do not stop bleeding or will not heal also merit examination by a skin care professional.
When the time comes to conduct the exam, the USNLM recommends following these steps:
- Look closely at your entire body, both front and back, in the mirror.
- Check under your arms and on both sides of each arm. Be sure to examine the backs of your upper arms, which can be hard to see.
- Bend your arms at the elbow, and examine both sides of your forearm.
- Examine the tops and palms of your hands.
- Examine the front and back of both legs.
- Examine your buttocks and between your buttocks.
- Examine your genital area.
- Examine your face, neck, the back of your neck, and scalp. Use both a hand mirror and full-length mirror, along with a comb, to see areas of your scalp.
- Examine your feet, including the soles and the spaces between your toes.
- Ask a person you trust to help examine hard-to-see areas.
Skin cancer poses a formidable threat, but many cases of the disease are preventable. Routine skin self-exams are a vital component of skin cancer prevention. TF256909
-

 NEWS3 years ago
NEWS3 years ago2 hurt, 1 jailed after shooting incident north of Nocona
-

 NEWS2 years ago
NEWS2 years agoSuspect indicted, jailed in Tia Hutson murder
-

 NEWS2 years ago
NEWS2 years agoSO investigating possible murder/suicide
-

 NEWS2 years ago
NEWS2 years agoWreck takes the life of BHS teen, 16
-
 NEWS2 years ago
NEWS2 years agoMurder unsolved – 1 year later Tia Hutson’s family angry, frustrated with no arrest
-

 NEWS2 years ago
NEWS2 years agoSheriff’s office called out to infant’s death
-

 NEWS2 years ago
NEWS2 years agoBowie Police face three-hour standoff after possible domestic fight
-

 NEWS3 years ago
NEWS3 years agoDriver stopped by a man running into the street, robbed at knifepoint






